Wound healing is often described as a progressive biological process. In reality, it is very dynamic, often broken by microscopic disturbances which are not visible on the surface. Biofilm formation is one of these disruptions that have become one of the most enduring and most underestimated clinical challenges. It alters the wound environment in ways that conventional assessment can easily overlook.
Biofilm as a Structural Defense System
Biofilm is not merely a brood of bacteria. It is a microbial community that is encased in a self-produced extracellular matrix. This matrix is a physical and chemical barrier, making antibiotics ineffective and hindering immune cells. When established, it acts as a living tissue rather than a loose infection, hence is resilient to chronic wounds.
The most difficult aspect of biofilm is that it alters the behavior of bacteria. Microorganisms in this structure settle in a slower metabolic condition and this reduces their vulnerability to antimicrobial agents. This change establishes a survival plan that will last long and cannot be easily interfered.
When Healing Becomes Stagnation
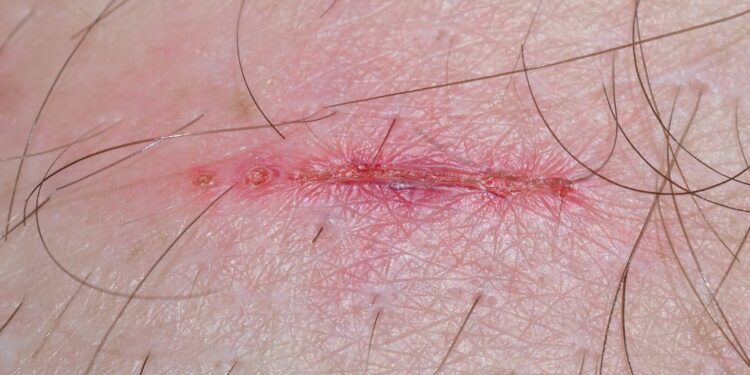
A biofilm-affected wound does not always appear dramatically infected. Rather, it tends to appear as a non-progressive clinical presentation. Healing plateaus, exudate persists, and granulation tissue formation becomes inconsistent. This deceptive stability can delay escalation of care.
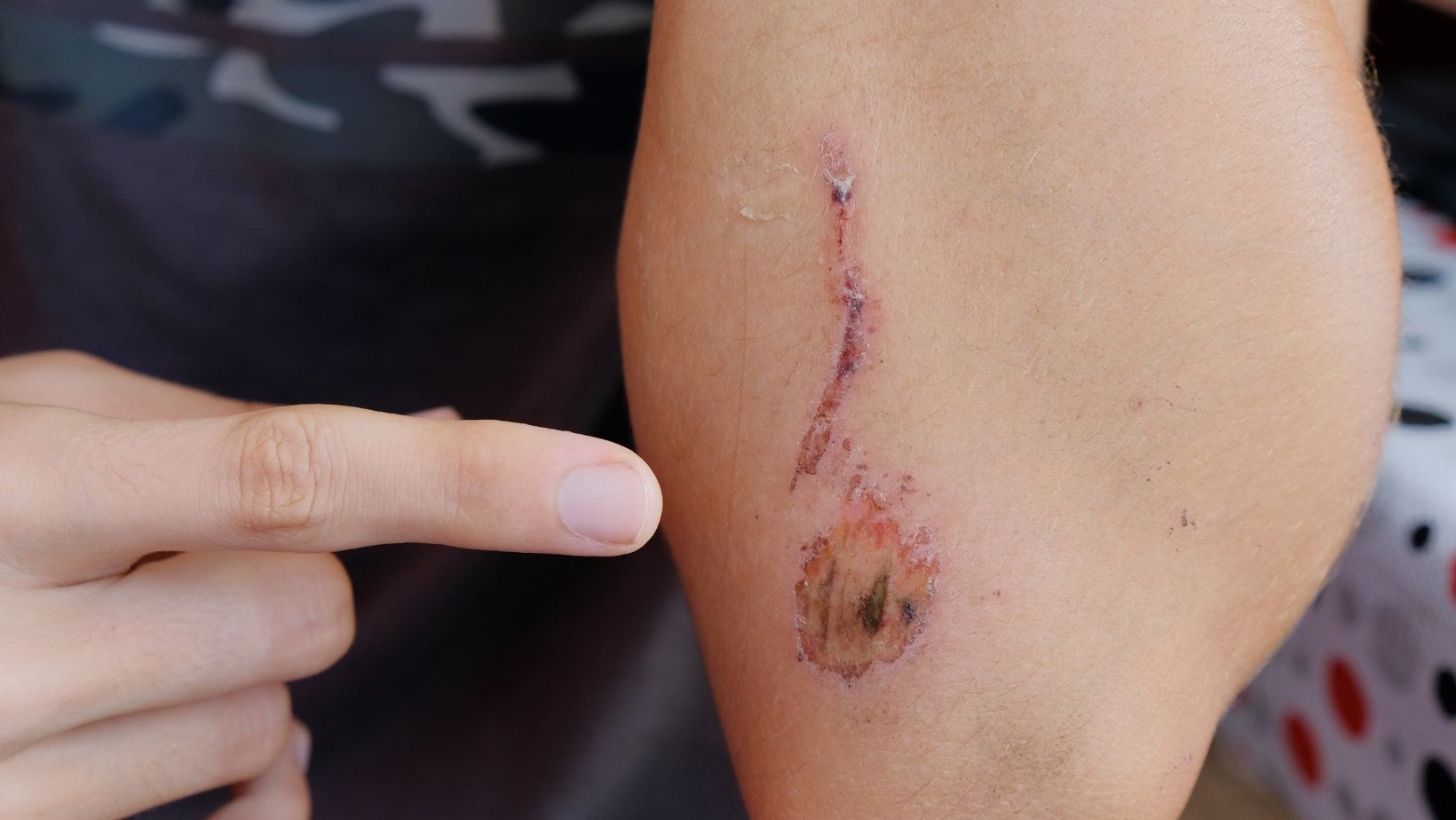
In practice, this means that a wound may appear “stable but not improving” for extended periods. This pattern is one of the most important clinical clues. It reflects an underlying biological interference rather than a simple delay in recovery.
Environmental Conditions That Favor Persistence
Biofilm development is strongly influenced by the wound environment. Moisture imbalance, necrotic tissue, and repeated contamination provide an environment that is conducive to microbial adherence and growth. Once developed, the structure is self-sustaining.
Certain clinical scenarios increase susceptibility. For example, severe burn injuries create large areas of exposed tissue with compromised barriers. This provides an ideal surface for microbial colonization. The extensive tissue damage and inflammatory response further complicate the body’s ability to regulate early bacterial growth.
The Challenge of Recognition in Clinical Settings
One of the significant difficulties in managing biofilm-associated wounds is identification. Typical indicators of infection are usually dampened or missing. Rather, clinicians have to use indirect evidence like stagnant healing processes and repeated inflammation despite proper treatment. Understanding wound care for patients is an important aspect in this regard.
Disruption as a Core Strategy
Effective management requires physical and chemical disruption of the biofilm structure. Debridement is also a key procedure since it removes not only necrotic tissue but some of the microbial matrix as well. However, individual interventions seldom suffice. Re-establishment can easily be prevented by repeated disruption.
Adjunct therapies are increasingly becoming popular to augment outcomes. Topical antimicrobials designed for penetration into biofilm structures can improve treatment response. In selected cases, systemic support may also be required to optimize overall healing conditions.
Physiological Support and Recovery Dynamics
Wound healing is not solely a local process. Recovery trajectories are also greatly influenced by systemic physiological factors. Oxygenation of tissues is of specific significance as oxygen aids cell repair processes and immunity. Oxygen therapy is also applied in certain clinical conditions to maximize oxygen delivery to injured tissue and increase the overall healing capacity.
Metabolic status, circulation, and immune competence all interact with local wound conditions. When these systems are impaired, biofilm-associated wounds become even more resistant to resolution.
Endnote
Biofilm formation is a structural obstacle and not mere infection. It must be handled through persistence, multi-level interventions, and re-evaluation. With a growing clinical insight, treatment methods are slowly shifting toward more specific and disruption-oriented modes of treatment.









Discussion about this post