Glioblastoma is an aggressive brain tumor, and treatment decisions often need to be made quickly. Because it can affect areas responsible for movement, speech, memory, and behavior, each stage of care — from diagnosis to surgery and follow‑up — benefits from a center with strong neuro‑oncology expertise.
Germany’s mix of advanced imaging, specialized neurosurgery, and coordinated oncology care draws many international patients. Some families also ask about alternative approaches, but their relevance depends on the medical details of each case.
This guide provides background information. Final decisions should be made in consultation with the treating team.
Why Glioblastoma Requires Specialized Neuro-Oncology Centers
Glioblastoma often grows in areas of the brain that control essential functions. Surgeons can’t simply “take wide margins” the way they might with tumors elsewhere in the body. Many lesions sit close to regions responsible for speech, movement, or memory. It means every surgical decision carries functional consequences. Experienced centers rely on high‑resolution imaging, functional mapping, and intraoperative monitoring to remove as much tumor as possible while preserving the patient’s abilities.
Treatment doesn’t end in the operating room. Radiotherapy, systemic therapy, pathology, and molecular testing all need to be coordinated, and this works best when handled by a team that communicates closely — neurosurgeons, oncologists, radiologists, pathologists, rehabilitation specialists, and supportive‑care professionals. When they work as a unit, patients receive a coherent plan rather than a collection of separate opinions.
Rehabilitation and symptom support start early. Fatigue, seizures, cognitive shifts, and mobility changes often appear soon after diagnosis, so having specialists who can respond quickly matters. Centers that build neuro‑rehabilitation into routine care help patients stay functional throughout treatment.
Diagnosis and Treatment Planning — What Must Be Confirmed First
Before discussing treatment options, doctors must verify the diagnosis and understand the tumor’s location and biology. These early steps ensure that the plan is based on accurate information.
Imaging and Differential Diagnosis
MRI with contrast is the primary way to understand how a suspected glioblastoma behaves and interacts with nearby brain structures. Specialists usually compare current scans with earlier ones to see how the cancer has evolved. It helps distinguish glioblastoma from other similar conditions and guides decisions about whether surgery is possible.
Pathology and Molecular Profiling
The diagnosis is only confirmed after neuropathology examines the tumor tissue. Identifying the exact tumor type and assessing key molecular markers, such as MGMT promoter status or IDH mutation, helps the team understand prognosis and choose appropriate treatment options. These findings don’t dictate a single plan, but they shape how therapy is tailored.
Multidisciplinary Tumor Board
Most specialized hospitals discuss glioblastoma cases at a multidisciplinary neuro-oncology board, where relevant specialists review the case together. That avoids one‑sided decisions and ensures that surgery, systemic therapy, and supportive care are aligned. For patients, it means the plan reflects the combined judgment of several doctors.
Key Criteria Patients Can Use to Choose a Glioblastoma Center in Germany
When patients compare clinics for glioblastoma treatment in Germany, they usually look past general hospital rankings and focus on whether the team truly handles complex neuro‑oncology cases. A few practical markers help with that:
- Neurosurgeons with a clear neuro‑oncology focus. Glioblastoma surgery requires dedicated expertise. Many patients begin by reviewing profiles of leading neurosurgeons in Germany for brain tumors, to understand the level of experience.
- Regular work with difficult tumor locations. Centers that operate near speech, motor, or memory areas every week are better prepared to balance resection and function.
- Modern navigation and monitoring. Neuronavigation, mapping, and intraoperative monitoring support maximal safe removal.
- Reliable neuropathology and molecular testing. Accurate MGMT, IDH, and other markers depend on strong pathology labs.
- Integrated radiotherapy and neuro‑oncology services. Postoperative treatment moves fast; close coordination avoids delays.
- A capable neuro‑ICU. Early recovery is fragile, and organized complication‑management pathways matter.
- Early rehabilitation and cognitive support. Helps patients stay functional throughout treatment, not only afterward.
- Clear communication for international patients. Structured coordination and accessible reports make the process far easier for families traveling from abroad.
Surgery and “Maximal Safe Resection” — What This Means
Neurosurgery for brain tumors in Germany is often the first major step in glioblastoma care when the tumor can be reached without putting essential functions at unacceptable risk. The goal isn’t simply to remove what’s visible, but to take out as much tumor as possible while preserving speech, movement, and other key abilities.
Experienced teams use tools like neuronavigation, intraoperative imaging, and functional monitoring to stay oriented during surgery and avoid critical pathways. Still, some tumors can’t be fully or safely removed — location, the patient’s condition, and the risk to speech or movement set the limits.
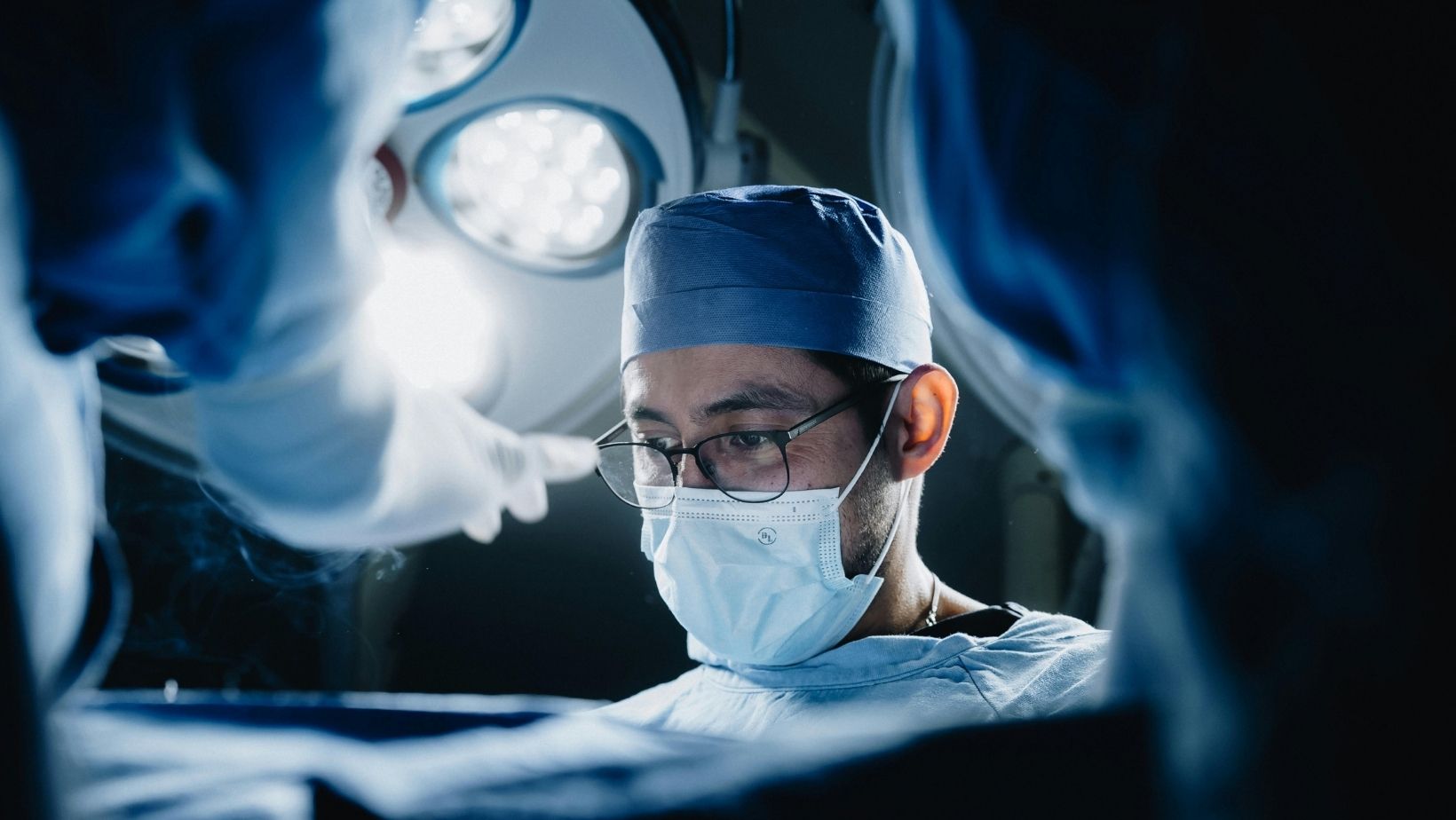
If surgery is reduced or not possible, treatment continues based on imaging and biopsy results. Radiotherapy, systemic therapy, and supportive care are coordinated from the start so the plan can move forward without delay.
Where Immunotherapy-Type Options May Enter the Conversation
Before discussing any non‑standard or innovative options, it helps to be clear about where they actually fit in glioblastoma care. They don’t replace established treatment, but in certain situations — depending on the diagnosis and the patient’s condition — they may become part of the discussion.
Clinical Trials and Individualized Approaches
Clinical trials remain the primary way to access new treatments for glioblastoma. They offer structured monitoring, though eligibility varies. In some cases, doctors may also discuss individualized immunotherapy options for glioblastoma that use a patient’s own cells, but whether they make sense depends entirely on the specifics of the diagnosis.
When Surgery Is Not Feasible or Not Recommended
If the tumor sits in a critical area or surgery carries too much risk, treatment shifts to non‑surgical options such as radiotherapy, systemic therapy, and, in selected situations, immunotherapy‑type strategies.
It is also where dendritic cells as alternative to surgery, may be mentioned. They aim to stimulate the immune system using tumor‑specific antigens, but their role remains investigational. Here, “alternative” means an option when surgery cannot be done safely, not a substitute for surgery when it is appropriate.
How to Evaluate Claims Safely
Any treatment that promises guaranteed results deserves caution. It’s reasonable to ask about evidence, monitoring, risks, and how the approach fits into the overall plan. Reputable centers explain the benefits and limitations and do not steer patients away from standard therapy without a documented medical reason.
Practical Steps for International Patients
Most centers follow a similar routine when working with international patients. The first steps usually look like this:
- Gather your medical files. Recent MRI scans in DICOM format, radiology reports, pathology results, and a brief treatment summary help the team review your case quickly.
- Request a multidisciplinary review or second opinion. Many hospitals can look at your scans and reports remotely, so neurosurgeons, oncologists, and radiologists can align their recommendations before you decide to travel.
- Clarify the treatment sequence and timeline. Ask what the first days and weeks will involve — repeat imaging, possible surgery dates, radiotherapy planning, and how long you may need to stay.
- Plan travel and basic logistics. Depending on the plan, you may need to remain in Germany for several days or weeks. Sorting out accommodation and support early makes things easier.
- Discuss follow‑up and remote communication. After returning home, part of your care can often continue remotely. Confirm how to send new scans and who your main contact will be.
Questions to Ask Before Choosing a Center
Patients often feel more confident when they know what to ask when choosing a neurosurgeon for glioblastoma. The following questions guide discussions with potential centers:
- What diagnosis has been confirmed, and does anything require re‑evaluation?
- Will a multidisciplinary tumor board review the case?
- What is the surgical goal, and what functional risks are expected?
- What technologies are used for mapping and intraoperative monitoring?
- How will postoperative radiotherapy and systemic therapy be coordinated?
- Are clinical trials available, and what determines eligibility?
- What rehabilitation and neurocognitive support are offered?
- How will complications be managed if they occur?
- What follow‑up schedule is recommended?
- What documents are needed for a full review?
- What is the expected timeline for starting treatment?
Conclusion
Choosing a glioblastoma center in Germany is less about hospital names and more about how well the team handles complex neuro‑oncology cases, and how coordinated the care actually is. Innovative or immune‑based options may come up in specific situations. Still, they only make sense when weighed against established treatment.
For international patients, having complete medical files and a clear idea of the likely treatment steps makes the process smoother. It helps plan the trip with fewer surprises.
FAQ
How do patients choose a glioblastoma center in Germany?
They focus on the team’s neuro‑oncology experience, the surgeons’ track record, and the coordination of the different parts of treatment.
Is surgery always required for glioblastoma?
Surgery is considered when it is safe and feasible, but some tumors cannot be fully or safely removed. In such cases, the team plans treatment based on imaging, biopsy, and functional risks.
Are immunotherapy options available for glioblastoma?
Some centers offer clinical trials or individualized approaches, but these are considered selectively. Eligibility depends on tumor features, prior treatments, and overall health.
What documents do international patients need to prepare?
MRI scans, pathology reports, molecular testing, and treatment history are typically required. These help the team understand the case and plan the next steps.
References
- Duffau H. Surgery of diffuse gliomas: new concepts and technical advances. Nature Reviews Neurology. 2020.
- Dr. Ahmed F. & Dr. Volvak M. Ranking 5 Leading Neurosurgeons in Germany for Brain Tumor. Airomedical. Updated 2026.
- Binder Z.A., Berger M.S. Functional mapping and awake surgery for gliomas in the eloquent cortex. Neurosurgery. 2022.
- Kozina J. & Dr. Volvak A. Dendritic Cell Cancer Therapy Guide. Airomedical. Updated 2025.
- Lim M., Xia Y., Bettegowda C., Weller M. Immunotherapy for glioblastoma: moving toward combination strategies. Nature Reviews Clinical Oncology. 2022.
- Batich K.A., Mitchell D.A. Dendritic cell vaccines for glioblastoma: progress, challenges, and next steps. Neuro‑Oncology Advances. 2023.












Discussion about this post