The infrastructure for drug screening sits in the background of most modern clinical research, but it is doing more work than the protocols make visible. Clinical trials, particularly those investigating compounds that interact with substances of abuse or that recruit populations with prior or concurrent substance use, depend on reliable screening tools at multiple points in the patient pathway. Inclusion eligibility, baseline characterisation, ongoing monitoring during the active phase, and post-trial follow-up all rely on quick, validated, repeatable screens.
The pressure on screening infrastructure has grown sharply with the resurgence of psychedelic medicine, ketamine-assisted protocols, and other research domains that intersect with controlled substances. The National Institute on Drug Abuse has emphasised the importance of robust monitoring infrastructure in any research program operating in this space, and the practical translation of that guidance is that research sites need access to consistent, accurate, cost-controlled screening at scale.
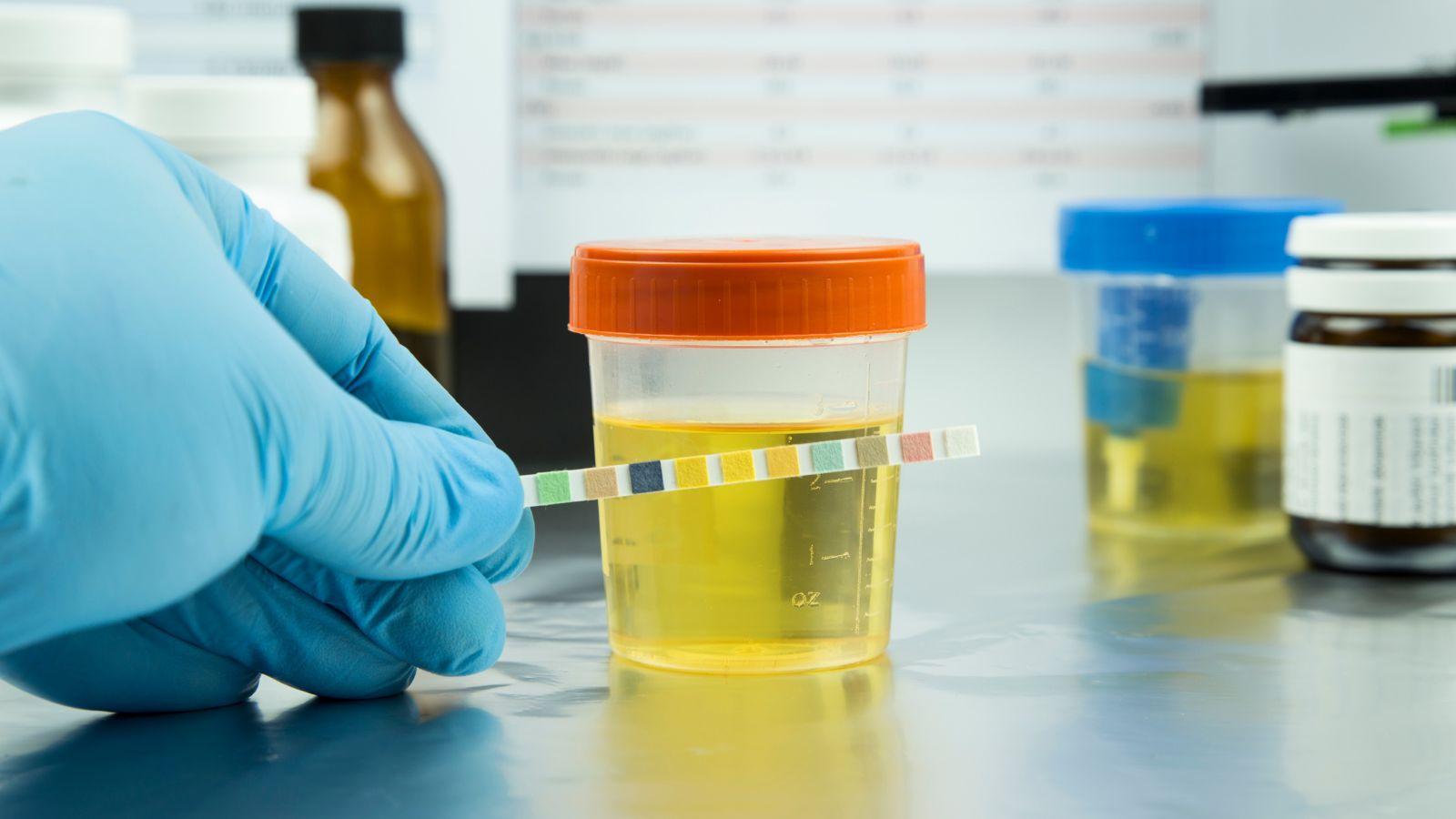
Suppliers offering Discounted Drug Tests have become an operational backbone for many sites running these protocols. Multi-panel cup tests provide the rapid, point-of-care screening layer that supplements deeper analytical work, and the cost difference between a properly priced point-of-care screen and a full laboratory assay is significant when multiplied across a trial with several hundred participants screened multiple times each.
The clinical research case for this layered approach is well established. Point-of-care screens at the eligibility stage filter the population efficiently. Periodic monitoring screens during the active phase catch protocol deviations early without consuming the analytical budget. Confirmatory laboratory work happens only when the point-of-care screen flags something worth investigating. The result is a screening pipeline that protects data quality without inflating the per-participant cost.
There is also a participant experience dimension that gets underweighted. Point-of-care testing returns results in minutes, which means participants are not left waiting on sensitive eligibility decisions for days. That speed matters in trials that recruit populations with significant logistical or psychological friction around the research process. A faster screening turnaround reduces dropout between consent and dosing.
For research programs operating at the leading edge of contemporary therapeutics, screening infrastructure is no longer a back-office concern. It is part of the protocol design.
FAQ
Are point-of-care drug tests accepted in clinical research? Yes. They are widely used as initial screening tools, with laboratory confirmation reserved for results that require analytical certainty.
How does point-of-care screening compare to laboratory assays? Point-of-care screens are faster and lower cost. Laboratory assays provide quantitative precision and legal-grade evidence. Most research designs use both in sequence.
What does discounted bulk pricing typically cover? Bulk and promotional pricing usually applies to standard multi-panel cup configurations purchased for institutional or research use.
Are point-of-care results documented in the case report form? Yes. Most protocols capture point-of-care results as initial screen data, with confirmatory analytical results documented separately when applicable.












Discussion about this post